© Borgis - Postępy Nauk Medycznych 4/2017, s. 218-222
*Jan Sobstyl1, Michał Sojka1, Krzysztof Pyra1, Andrzej Wolski2, Radosław Krupiński2, Tomasz Jargiełło1
Endovascular treatment of abdominal aortic aneurysm with a short proximal neck using endoanchors – case report
Wewnątrznaczyniowe leczenie tętniaka aorty brzusznej o krótkiej proksymalnej szyi przy użyciu wewnątrznaczyniowych wkrętów – opis przypadku
1Department of Interventional Radiology and Neuroradiology, Medical University in Lublin
Head of Department: Professor Małgorzata Szczerbo-Trojanowska, MD, PhD
2Department of Vascular Surgery, University Hospital No. 4 in Lublin
Head of Department: Andrzej Wolski, MD, PhD
Streszczenie
Leczenie wewnątrznaczyniowe tętniaków aorty brzusznej (TAB) wciąż stanowi duże wyzwanie terapeutyczne w przypadku występowania niekorzystnych cech anatomicznych proksymalnej szyi tętniaka. Mimo że w porównaniu do otwartej operacji naprawczej leczenie wewnątrznaczyniowe TAB cechuje się zmniejszoną śmiertelnością okołooperacyjną, ilość reinterwencji jest wciąż wyższa po leczeniu wewnątrznaczyniowym. Jedną z głównych przyczyn jest zwiększone ryzyko wystąpienia zacieku typu Ia i/lub migracji stentgraftu w związku z obecnością niekorzystnych cech anatomicznych proksymalnej szyi tętniaka. Spośród wielu technik leczenia stosowanych w powyższym przypadku, wyniki mocowania stentgraftu przy użyciu wkrętów wewnątrznaczyniowych wydają się szczególnie obiecujące. Założeniem tej metody jest połączenie zalet małoinwazyjnego leczenia wewnątrznaczyniowego z trwałością otwartej operacji naprawczej. Celem pracy jest przedstawienie opisu przypadku leczenia objawowego pacjenta z niepękniętym TAB o krótkiej proksymalnej szyi, przy użyciu wkrętów wewnątrznaczyniowych.
Summary
Endovascular treatment of the abdominal aortic aneurysm in case of adverse anatomical features of the proximal aneurysmal neck, still represents a major therapeutic challenge. Although, endovascular aortic repair (EVAR) compared to open surgery repair is characterized by a reduced perioperative mortality, the reintervention incidence after EVAR is still higher than after open surgery repair. One of the main reason of that result is an increased risk of type Ia endoleak development and/or the stentgraft migration after the endovascular treatment when unfavorable anatomy is present. From among many of techniques which are used in the treatment of AAA with a “hostile neck” anatomy, the results of the stentgraft fixation with the endoanchors seem to be particularly encouraging. The assumption of this technique is to combine the advantages of minimally invasive endovascular procedure with the durability of an open surgery repair. The aim of this article is to report the case of the successful endovascular treatment of symptomatic, unruptured abdominal aortic aneurysm with a short proximal neck using endoanchors.

Introduction
Abdominal aortic aneurysm (AAA) is a localized enlargement of the abdominal aorta to the diameter ≥ 30 mm. The prevalence of AAA is estimated to 1.3-12.5% in men and 0-5.2% in women. AAA formation known risk factors are age (prevalence significantly increases with age, especially > 65 years old), male, family history of AAA, smoking, hypercholesterolemia and hypertension (1, 2). Unruptured AAA symptoms may include atypical abdominal or back pain, and sometimes a palpable pulsatile abdominal mass. However, in most cases a course of the disease is asymptomatic until rupture of AAA. Then an acute abdominal pain and shock usually occur.
According to the European Society of Cardiology Guidelines on the diagnosis and treatment of aortic diseases from 2014, ultrasonography (US) is a recommended AAA screening examination. Screening for AAA with US is recommended in all men > 65 years of age, may be considered in woman > 65 years of age with a history of tobacco smoking. CT and MRI are the reference methods for pre- and postoperative assessment of AAA. Aortography may be a useful imaging modality, if CT and MRI results are unclear and ambiguous.
AAA repair is indicated if it’s diameter exceeds 55 mm or an aneurysm growth exceeds 10 mm/year (3). Although endovascular aortic repair (EVAR) is a safe, effective, and currently the most widely used AAA treatment method, there are still issues which need to be resolved to significantly improve this treatment (4). EVAR compared to open surgery repair is characterized by a reduced perioperative mortality, but the reintervention incidence after EVAR is still higher than after open surgery repair. Additionally, results of many studies indicate that the difference in mortality rate between EVAR and open surgery is reduced in a few years after the treatment (5). Successful endovascular treatment depends largely on the anatomical factors. The presence of an unfavorable anatomy like proximal aneurysmal neck length < 10 mm, diameter > 28 mm and angle > 60 degrees, conical shape, calcification or thrombus thickness > 2 mm covering > 180 degree of the circumference of the aorta belong to the adverse anatomical features. This challenging proximal aortic neck anatomy is called a “hostile neck”. This condition reduces the efficacy of endovascular treatment and predisposes to the stentgraft migration and/or increases the risk of type Ia endoleak development, blood inflow between the stentgraft and the aortic wall in the proximal landing zone (6, 7).
A variety of techniques are used in the treatment of AAA with a “hostile neck” anatomy. In order to adjust to the anatomical variability a suprarenal bare stents, stentgrafts with barbs and hooks, fenestrated stentgrafts, chimney graft technique or polymer-injected sealing rings have been deployed over the years (8, 9).
The idea of combining the advantages of minimally invasive endovascular procedure with the durability of an open surgery repair has led to the emergence of endovascular staples, also called endoanchors. The endoanchor objective is to tack the stentgraft through all three layers of the aortic wall. The aim is to provide the durability of the stentgraft fixation similar to that obtained with a sutured anastomosis during open surgery repair (10).
Case report
AAA was detected accidentally during the ultrasound examination of the 64 years old patient. Initially the aneurysm diameter was approximately 40 mm. Surveillance US examination performed after the 6 and 12 months revealed an aneurysm diameter increase to 50 mm. Another US examination performed because of the emergence of an abdominal pain, further expansion of the sac to 65 mm in diameter and tenderness during the pressure with a probe was observed.
Patient was sent to a vascular surgeon and an urgent CT angiography was performed. Due to the systematic enlargement of the AAA sac and the presence of abdominal pain during physical examination the patient was qualified for urgent stentgraft implantation.
CT angiography revealed a short aneurysmal neck and a thrombus placed on the right and anterior side of the aortic wall just below the renal arteries, comprising approximately 40% of the circumference of the abdominal aorta (fig. 1a, b). Moreover, the CT angiography presented a thrombus defect (“thrombus ulceration”) on the anterior wall of the AAA and an aneurysmal dilatation of the right common iliac artery proximal to the iliac bifurcation with a diameter of approximately 28 mm harbouring a small mural thrombus (fig. 1c). There were no obvious imaging features of the aneurysm rupture.
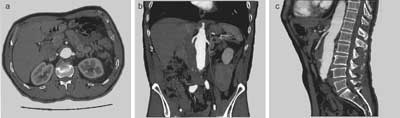
Fig. 1a-c. Images of CT angiography before the treatment: a) a thrombus visible just below the renal arteries on the right side of the abdominal aorta; b) a short length and a conical shape of the proximal aneurysmal neck; c) a thrombus defect visible on the anterior wall of the AAA in the sagittal projection
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Golledge J, Muller J, Daugherty A, Norman P: Abdominal aortic aneurysm. Pathogenesis and implications for management. Arterioscler Thromb Vasc Biol 2006; 26: 2605-2613.
2. Makrygiannis G, Labalue P, Erpicum M et al.: Extending abdominal aortic aneurysm detection to older age groups: preliminary results from the Liege screening programme. Vasc Surg 2016; 36: 55-63.
3. Erbel R, Aboyans V, Boileau C et al.: 2014 ESC Guidelines on the diagnosis and treatment of aortic diseases. Eur Heart J 2014; 35: 2905-2908.
4. Tina TN, Mirocha J, Magner D, Gewertz BL: Variations in the utilization of endovascular aneurysm repair reflect population risk factors and disease prevalence. J Vasc Surg 2010; 51: 801-809.
5. Patel R, Sweeting MJ, Powell JT et al.: Endovascular versus open repair of abdominal aortic aneurysm in 15-years’ follow-up of the UK endovascular aneurysm repair trial 1 (EVAR trial 1): a randomised controlled trial. Lancet 2016; 388(10058): 2366-2374.
6. Kopp R, Kasprzak PM: Commentary: are EndoAnchors up to the challenge of a hostile proximal neck? J Endovasc Ther 2015 Apr; 22(2): 171-173.
7. White SB, Stavropoulos SW: Management of Endoleaks following Endovascular Aneurysm Repair. Semin Intervent Radiol 2009; 26(1): 33-38.
8. Jordan WD, Mehta M, Ouriel K, Arko FR: One-year results of the ANCHOR trial of EndoAnchors for the prevention and treatment of aortic neck complications after endovascular aneurysm repair. Vascular 2016 Apr; 24(2): 177-186.
9. Verhoeven EL, Katsargyris A, Oikonomou K et al.: Fenestrated endovascular aortic aneurysm repair as a first line treatment option to treat short necked, juxtarenal, and suprarenal aneurysms. Eur J Vasc Endovasc Surg 2016 Jun; 51(6): 775-781.
10. Perdikides T, Melas N, Lagios K et al.: Primary endoanchoring in the endovascular repair of abdominal aortic aneurysms with an unfavorable neck. J Endovasc Ther 2012; 19(6): 707-715.
11. Antoniou GA, Georgiadis GS, Antoniou SA et al.: A meta-analysis of outcomes of endovascular abdominal aortic aneurysm repair in patients with hostile and friendly neck anatomy. J Vasc Surg 2013; 57(2): 527-538.
12. Ohki T, Deaton DH, Condado JA: Aptus Endovascular AAA Repair System. Endovasc Today 2006; 7: 29-36.
13. Deaton DH: Improving proximal fixation and seal with the HeliFx Aortic EndoAnchor. Semin Vasc Surg 2012; 25(4): 187-192.
14. Jordan WD, de Vries JP, Ouriel K, Mehta M: Midterm outcome of EndoAnchors for the prevention of endoleak and stent-graft migration in patients with challenging proximal aortic neck anatomy. J Endovasc Ther 2015; 22(2): 163-170.

